Please click the frequently asked questions below for further information and IPC precautions required:
-
What is Diphtheria?
Diphtheria is a highly contagious infection that affects the nose and throat, and sometimes the skin. It’s rare in the UK, but there’s a small risk of catching it if you travel to some parts of the world.
Diphtheria can be a serious illness and sometimes fatal, especially in children, if it’s not treated quickly. Vaccination can prevent it.
-
How does it spread?
Diphtheria is a highly contagious droplet spread bacterial infection. It’s spread by coughs and sneezes, or through close contact with someone who is infected.
You can also get it by sharing items, such as cups, cutlery, clothing or bedding, with an infected person.
The maximum incubation period for diphtheria is 10 days; however, there may be longer duration of carriage in asymptomatic carriers but there is little evidence. Therefore, close contacts should be identified from 10 days before onset of diphtheria symptoms in a case.
-
What are the symptoms of Diphtheria?
Symptoms usually start 2 to 5 days after becoming infected.
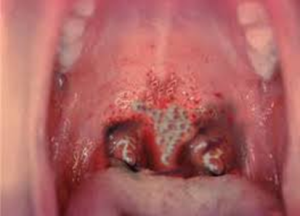
Symptoms of diphtheria include:
- a thick grey-white coating that may cover the back of your throat, nose and tongue
- a high temperature (fever)
- sore throat
- swollen glands in your neck
- difficulty breathing and swallowing
- In countries with poor hygiene, infection of the skin (cutaneous diphtheria) is more common.
If it’s cutaneous diphtheria, it can cause:
- pus-filled blisters on your legs, feet and hands
- large ulcers surrounded by red, sore-looking skin
-
Why is this important?
If NIAS staff are aware that the patient has a suspected or confirmed case this should be communicated to the Control Room (Emergency or Non-emergency as appropriate) and the staff in the receiving unit when transferring the patient to ensure effective patient care and management.
-
IPC Precautions
- Droplet precautions should be used
- Hand Hygiene should be completed as per the 5 moments in line with usual practice.
- Eye protection should be worn
- Fluid Resistant surgical mask should be worn
- Gloves and Aprons should be worn.
- The patient should be transported via ambulance with no other patients present.
- Laundry should be treated as contaminated, placed into an alginate bag and placed into a red laundry bag.
-
What cleaning is required?
All equipment and the ambulance should have an in-between patient clean paying particular attention to touch points.
-
Do staff need prophylaxis or follow up?
Immediate Actions: Inform Station Officer / Line Manager and contact the IPC team during working hours for further advice.
If appropriate PPE is worn then no follow up is required.
If a staff member following a risk assessment is deemed a close contact then prophylaxis will need to be considered and a risk assessment will be completed by Occupational Health.
Staff may be deemed as a close contact and should be considered for prophylaxis:
- This will depend on the presentation of diphtheria in the index case, which body sites were positive on swabbing, and what personal protective equipment (PPE) the HCW wore while attending the case and if there were any breaches in PPE.
- Respiratory cases, HCW who have given mouth to mouth resuscitation to or intubated the index case (without appropriate PPE) would normally be considered as close contacts
- Where eye protection has not been worn and droplet exposure has occurred (for example, a patient has coughed during the collection of a throat swab)
Each case will be individually risk assessed with the staff member, their line manager and the IPC team. If required a referral to Occupational Health will be made.




