Please click the frequently asked questions below for further information and IPC precautions required:
-
What is HFM?
Hand, foot and mouth disease is a common infection that causes mouth ulcers and spots on the hands and feet.
It’s most common in young children – particularly those under 10 – but can affect older children and adults as well. There’s no cure for it, so you have to let it run its course.
Hand, foot and mouth disease can be unpleasant, but it will usually clear up by itself within 7 to 10 days. You can normally look after yourself or your child at home.
The infection is not related to foot and mouth disease, which affects cattle, sheep and pigs.
-
Why is this information important?
If NIAS staff are aware that the patient has a suspected or confirmed case this should be communicated to the Control Room (Emergency or Non-emergency as appropriate) and the staff in the receiving unit when transferring the patient to ensure effective patient care and management.
-
How is it spread?
Someone with hand, foot and mouth disease is most infectious from just before their symptoms start until they’re feeling better.
The infection can be spread by close person to person contact and contact with contaminated surfaces.
The virus is found in:
- the droplets in the coughs and sneezes of an infected person – you can become infected if you get these on your hands and then touch your mouth, or if you breathe in the droplets
- an infected person’s faeces – if an infected person doesn’t wash their hands properly after going to the toilet, they can contaminate food or surfaces
- an infected person’s saliva or fluid from their blisters – you can become infected if this gets in your mouth
The infection is caused by a number of different viruses, so it’s possible to get it more than once. Most people develop immunity to these viruses as they get older.
-
What are the symptoms?
Thesymptoms of hand, foot and mouth disease usually develop between 3 and 5 days after being exposed to the infection.
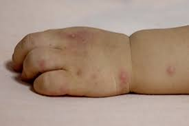
The first symptoms may include:
- a high temperature (fever), usually around 38°C to 39°C (100.4-102.2°F)
- a general sense of feeling unwell
- loss of appetite
- coughing
- abdominal (tummy) pain
- a sore throat and mouth
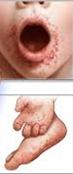
-
IPC Precautions
- Droplet precautions should be used.
- A fluid resistant surgical mask should be worn.
- Hand Hygiene should be completed as per the 5 moments in line with usual practice.
- Eye protection should always be risk assessed and used with any patient where there is a risk of splashes including spitting and productive coughing.
- Gloves and Aprons should be worn.
- The patient should ideally be transported via ambulance (eg. PCS) with no other patients present where possible. Individual cases can be discussed with the IPC team and a risk assessment can be made.
- Laundry should be treated as contaminated, placed into an alginate bag and placed into a red laundry bag.
-
What cleaning is required?
All equipment and the ambulance should have an in-between patient clean paying particular attention to touch points.
-
Do staff need any prophylaxis or follow up?
Staff do not need to be followed up. Staff should remain vigilant for symptoms.




