Please click the frequently asked questions below for further information and IPC precautions required:
-
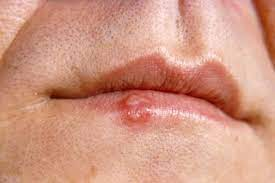
What is Herpes Simplex?
Thereare two types; type 1 and 2. They cause similar symptoms. Both have been found to cause cold sores, though type 1 is more common. Genital infection more often is caused by type 2. This pattern however is changing.
Consequences can be more serious if passed on to a baby during pregnancy or delivery.
As many as seven out of ten people become infected with herpes simplex of the mouth at some time during their life. Three out of four people when first infected (primary) will have very mild or even no symptoms and therefore will not seek any treatment. After or during
this primary infection the virus travels up from the skin to the nerve root.
Here it stays but can return to the skin from time to time (reactivate). This does not always happen. When it does, reactivation occurs often throughout life or may last for only a short period of time. Various things such as the common cold, sunlight or stress can trigger it.
-
Why is this information important?
If NIAS staff are aware that the patient has a suspected or confirmed case this should be communicated to the Control Room (Emergency or Non-emergency as appropriate) and the staff in the receiving unit when transferring the patient to ensure effective patient care and management.
-
How is it spread?
A person is most infectious to others when a sore has developed.
Usually this is through direct skin-to-skin contact, particularly with the vesicle, including kissing.
Many treatments (not cures) are available, though responses to them vary greatly.
-
What are the symptoms?
A small number of people have repeated outbreaks which can range from ‘very painful’ to just ‘a nuisance’. People often report an itching/tingling or a burning feeling before seeing a small group of red bumps that eventually blister. These then dry and form a yellow crust, which falls off within two weeks.
-
IPC Precautions
- Contact Precautions should be used until the blister is dry and crusted.
- Hand Hygiene should be completed as per the 5 moments in line with usual practice.
- Eye protection should be risk assessed
- Gloves and Aprons should be worn.
- The patient should be transported via ambulance with no other patients present where possible.
- Laundry should be treated as contaminated, placed into an alginate bag and placed into a red laundry bag.
-
What cleaning is required?
All equipment and the ambulance should have an in-between patient clean paying particular attention to touch points.
-
Do staff need any prophylaxis or follow up?
There is no follow up required.




