Please click the frequently asked questions below for further information and IPC precautions required:
-
What is Lyme disease?
Lyme borreliosis or Lyme disease is a zoonotic infection caused by the bacterium Borrelia burgdorferi and is transmitted to humans through the bite of an infected tick.
Ticks are small spider-like creatures that are found on bushes and undergrowth in countryside, parks and gardens. They feed on the blood of birds and mammals, including humans. If a tick bites an animal carrying Borrelia burgdorferi, the tick can also become infected and then transfer the bacteria to a human by biting them.
Most tick bites do not transmit Lyme disease and prompt, correct removal of the tick reduces the risk of transmission. It is estimated that the risk of symptomatic infection after being bitten is 1 to 5% in Europe.
-
How does it spread?
It is spread via tick bites. There is no evidence of transmission between humans.
-
What are the symptoms of Lyme disease?
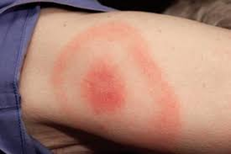
Many people with early-stage Lyme disease develop a distinctive circular rash (known as erythema migrans) at the site of the tick bite, usually around 3 to 30 days after being bitten.
Some people also experience flu-like symptoms such as:
- Fatigue
- muscle pain
- joint pain
- headaches
- fever
- chills
- neck stiffness
Late-stage disease can develop months or even years later if Lyme disease is left untreated or if treatment is delayed. Presentations may include inflammatory arthritis, nerve problems (numbness, limb pain, facial palsy and memory problems), cardiac problems, encephalitis and meningitis. A small number of people develop long-term health problems similar to fibromyalgia or chronic fatigue syndrome.
-
Why is this important?
If NIAS staff are aware that the patient has a suspected or confirmed case this should be communicated to the Control Room (Emergency or Non-emergency as appropriate) and the staff in the receiving unit when transferring the patient to ensure effective patient care and management.
-
IPC Precautions
- Standard Precautions should be used.
- Hand Hygiene should be completed as per the 5 moments in line with usual practice.
- Eye protection should be risk assessed for any concern regarding a splash risk.
- Gloves and Aprons should be risk assessed and worn if contact with the patient’s blood or bodily fluids.
- Laundry should be treated as per usual local policy.
-
What cleaning is required?
All equipment and the ambulance should have an in-between patient clean, paying particular attention to touch points.
-
Do staff need prophylaxis or follow up?
No staff follow up required.




