Please click the frequently asked questions below for further information and IPC precautions required:
-
What is Rubella?
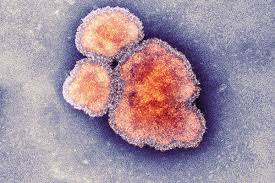
Rubella virus is a type of togavirus and causes rubella infection, also known as German measles and 3-day measles. Infections in otherwise healthy individuals are usually mild and self-limiting.
Rubella infection in pregnancy is a major concern as it can cause miscarriage or congenital rubella syndrome (CRS). CRS can cause severe birth defects if rubella is contracted before 20 weeks gestation and the earlier in the pregnancy, the greater the risk of complications.
-
How does it spread?
Rubella is transmitted primarily through direct or droplet contact from nasopharyngeal secretions. Humans are the only natural hosts. In temperate climates, infections usually occur during late winter and early spring.
The incubation period is 14 to 21 days, with the majority of individuals developing a rash 14 to 17 days after exposure. Individuals with rubella are infectious from one week before symptoms appear to four days after the onset of the rash.
Vertical (Maternal to foetal) transmission is a primary route of transmission in pregnancy.
-
What are the symptoms of Rubella?
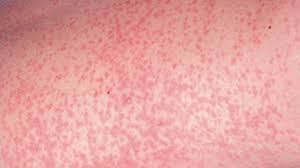
Signs and symptoms include:
- Rash (which typically lasts 3 days and starts on the face then progresses to trunk and limbs)
- Sore throat
- Fever
- Conjunctivitis
- Lymphadenopathy (which may last for several weeks)
- Arthralgia
Complications are rare, but include testicular swelling, thrombocytopenia, arthritis and in severe cases, post-infectious encephalitis, which can be fatal.
-
Why is this important?
If NIAS staff are aware that the patient has a suspected or confirmed case this should be communicated to the Control Room (Emergency or Non-emergency as appropriate) and the staff in the receiving unit when transferring the patient to ensure effective patient care and management.
-
IPC Precautions
- Droplet Precautions should be used.
- Hand Hygiene should be completed as per the 5 moments in line with usual practice.
- Eye protection should be worn.
- A Fluid Resistant Surgical Mask should be worn.
- Gloves and Aprons should be worn. Consider the use of a long sleeved gown if there will likely be prolonged contact with patient such as for personal care.
- The patient should be transported via ambulance with no other patients present.
- Laundry should be treated as contaminated, placed into an alginate bag and placed into a red laundry bag.
-
What cleaning is required?
All equipment and the ambulance should have an in-between patient clean paying particular attention to touch points.
-
Do staff need prophylaxis or follow up?
Staff should inform their line manager and the IPC team at the earliest time able during working hours.
If appropriate PPE has been worn then no follow up is required.
If you have been exposed to a patient with Rubella including the 7 days prior to onset of the rash, and appropriate PPE has not be worn or if there has been a breach, you will be referred to Occupation Health for a Risk assessment.
If the staff member is pregnant they should contact Occupational Health as soon as they are aware of the exposure.
- Links to guidance




